Most people over 60 religiously consume certain "bone-building" foods, convinced they're doing everything right. But emerging research reveals that some of the most recommended calcium sources might actually be working against your bone density — and the food't eager to share this inconvenient truth.
The Breakfast Staple That Blocks Calcium Absorption
It's the morning routine millions follow religiously — a bowl of fortified cereal with milk, believing they're loading-building calcium. But here's what the cereal companies don't advertise: many fortified cereals contain compounds that actually prevent your body from absorbing the calcium you think you're getting.

This means you could be consuming 300-400mg of calcium at breakfast and only absorbing a fraction of it, leaving yourving despite your best efforts. The culprit is often excess iron and zinc added to cereals, which compete directly with calcium for absorption in your intestines. It's like trying to push three people through a door at once — something gets blocked. A better morning choice? Plainats with sliced almonds and a small amount of yogurt, which provides calcium without the absorption blockers. And this breakfast issue is just the beginning of what most people get wrong about calcium.
Why Your "Healthy" Smoothie Might Be Bone-Depleting
Green smoothies packed with spinach seem like the perfect calcium boost — after all, leafy greens are loaded with this bone-building mineral. What nutritionists rarely mention is that spinach contains high levels of oxalates, compounds that bind to calcium and make it nearly impossible for your body to use
You could drink a spinach smoothie with 200mg of calcium and absorb less than 10mg — worse than eating a piece of white bread for your bone health.

Oxalates essentially handcuff the calcium, escorting it straight through your digestive system without stopping to help your bones. theater — looks healthy but delivers nothing. Switch to kale, bok choy, or collard greens instead. These provide the same vitamins with much lower oxalate levels, letting your body actually use the calcium. But even among "safe" green, there's one that's particularly deceptive.
The Supplement That Steals From Your Skeleton
Most people over 60 pop calcium carbonate supplements religiously, often the chalky tablets that promise 500-600mg per dose. Here's the problem nobody talks about: calcium carbonate requires stomach acid to break down, but stomach acid production naturally decreases after age 50.

Without enough acid, these supplements pass through largely unabsorbed while potentially creating kidney stones from the excess calcium your body can't process. The unabsorbed calcium doesn't just disappear harmlessly — it can interfere with magnesium absorption, a mineral that's actually more critical for bone strength than calcium itself. Choose calcium citrate instead, which absorbs without requiring stomach acid, or better yet, focus on food sources combined with the right co-factors. The ir even worse when you discover what most people eat right after taking their calcium supplement.
Coffee's Hidden Attack on Your Calcium Stores
It's incredibly taking your calcium supplement with your morning coffee, thinking you're being efficient with your health routine. But caffeine actively pulls calcium from your bones and flushes it through your kidneys, essentially undoing the supplement you just swallowed.

Just one cup of coffee can cause you to lose 6mg of calcium, and you're drinking 3-4 cups daily, you're creating a net calcium deficit regardless of supplementation. The mechanism is straightforward: caffeine increases calcium excretion through urine while simultaneously reducing calcium absorption in your intestines. It's a double hit your bones can't afford. If you must have coffee, wait at least 2 hours after taking and consider reducing to one cup daily after age 60. But coffee isn't the only beloved beverage working against your bone health.
The "Healthy" Drink That Acidifies Your Bones
Orange juice fortified with calcium seems like a smart choice — you're getting vitamin C and added calcium in one convenient drink. What the marketing doesn't mention is that the high sugar content creates an acidic environment in your body that forces your bones to release calcium to neutralize the acid.

Your skeleton essentially becomes an antacid tablet, sacrificing its calcium stores to buffer the sugar-induced ac that "healthy" morning OJ. The process is called acid buffering, and your bones are your body's primary alkaline reserve. When blood becomes too acidic from sugar, your body automatically pulls calcium phosphate from bones to restore pH balance. Skip the juice and eat half an orange with a handful of almonds instead. You C without the bone-depleting sugar spike. This acid-alkaline balance issue extends to another breakfast favorite that surprises most people.
Yogurt's Dark Secret After Age 60
Yogurt marketing targets adults specifically, promising calcium and probiotics for bone health and digestion. But most commercial yogurts are loaded with added sugars — often 15-20 grams per serving — which triggers the same acid-buffering response that steals calcium from your bones.

The probiotics are often minimal in processed yogurts, while content rivals that of ice cream, creating inflammation that interferes with bone formation. Your body prioritizes blood sugar regulation over bone building, so the calcium in that yogurt gets overshadowed by the metabolic chaos from sugar processing. Choose plain Greek yogurt with no added sugars, and add your own berries for natural sweetness without the calcium-robbing effect. Most people skip this one completely, not realizing how their dinner choices affect morning calcium absorption.
Why Evening Meals Block Morning Calcium
Most people focus on getting calcium in the morning but pay no attention to what they ate the night before. High-protein dinners, especially red meat, create an acidic residue that your body is still processing 12-16 hours later, right when you're trying to absorb morning calcium.

This means your breakfast calcium being used to neutralize last night's dinner rather than building bone density. The sulfur-containing amino acids in animal proteins break down into sulfuric acid, which your kidneys must buffer by pulling calcium from bones and flushing it through urine. Balance evening proteins with alkalizing vegetables like broccoli or Brussels sprouts, which help neutralize acid without sacrificing bone calcium. But protein timing isn't the only dinner mistake affecting your bone health.
The Mineral That Cancels Out Calcium Completely
Many people dutifully take calcium supplements but ignore magnesium, not realizing these minerals work as partners. Without adequate magnesium, calcium can't be properly utilized by bones and instead gets deposited in soft tissues like arteries and kidneys.

You could be consuming 1200mg of calcium daily, butnesium deficient, you're essentially building kidney stones instead of bone density. Magnesium activates the enzymes necessary for calcium absorption and helps convert vitamin D into its active form. Without it, calcium becomes metabolically useless and potentially harmful. The ideal ratio is 2:1 calcium to magnesium, but most people get a 4:1 or a dangerous imbalance. This mineral partnership extends to another nutrient that most people over 60 are unknowingly deficient in.
The Vitamin That Makes Calcium Disappear
Taking calcium without adequate vitamin D is a door without the key — the calcium simply can't get where it needs to go. Most adults over 60 have insufficient vitamin D levels, especially those living in northern climates or spending most time indoors.

Without enough vitamin D, your body can only absorb about 10-15% of the calcium you consume, rendering most dietary calcium useless for bone building. Vitamin D acts as a transport mechanism, helping calcium move from your digestive system into your bloodstream and ultimately into your bones. Without it, calcium gets excreted as waste. The recommended 600 IU for seniors is often insufficient — many need 1000-2000 IU daily, but this should be determined through blood testing. But even perfect vitamin D levels won't help if you're making this common timing mistake.
Why Taking Calcium All at Once Backfires
Most people take their entire daily calcium dose in supplement, thinking they're being efficient with their nutrition routine. Your body can only absorb about 500mg of calcium at one time — anything beyond that gets wasted and potentially causes digestive issues.

Taking a 1000mg calcium tablet is like trying to drink from a fire hose — most of it goes right past where it's needed. The absorption mechanism becomes saturated, and excess calcium can interfere with iron and zinc absorption, creating other nutritional deficiencies that affect bone health indirectly. Split your calcium into smaller doses throughout the day, or better yet, focus on getting 200-300mg from food sources at each meal. This timing issue becomes even more critical what most people eat alongside their calcium.
The Fiber That Blocks Bone Building
Whole grains are heavily promoted for senior health, but the timing of fiber intake can interfere with calcium absorption. High-fiber foods contain compounds called calcium in your digestive system, preventing absorption just like oxalates do.

Eating a high-fiber meal with calcium-rich foods can reduce calcium absorption by up to 50%, essentially cutting your bone-building nutrition in half. The phytates act like molecular magnets, attracting minerals and escorting them out of your body before they can be absorbed and utilized your high-fiber foods and calcium sources by 2-3 hours, or choose fermented grains like sourdough, which have lower phytate content. Doctors mention this often, but there's an even more surprising calcium blocker hiding in most medicine cabinets.
The Heartburn Medicationows Bones
Proton pump inhibitors (PPIs) for heartburn are among the most prescribed medications for people over 60. These acid-blocking medications prevent your stomach from producing the acid necessary to break down and absorb calcium from both food and supplements.
Long-term PPI use can reduce calcium absorption by up to 60%, significantly increasingture risk even when calcium intake appears adequate. The stomach acid these medications suppress is essential for converting calcium carbonate (the most common supplement form) into absorbable calcium ions. If you must use PPIs, switch to calcium citrate supplements and work with your doctor to find the lowest effective dose for the shortest duration possible. But even without PPIs, there's a common cooking method that destroys calcium availability.
How Overcooking Destroys Calcium in Vegetables
How Overcooking Destroys Calcium in Vegetables
A pot of overcooked, mushy broccoli next to fresh, bright green broccoli florets
Many seniors overcook vegetables, thinking softer foods are easier to digest and therefore healthier. Prolonged boiling or steaming can down the cellular structure that makes calcium bioavailable, essentially cooking the nutrition right out of your vegetables.

Overcooked calcium-rich vegetables can lose up to 70% of their absorbable calcium, turning nutritious greens into fiber with minimal bone-building value. The cell walls that contain calcium become so damaged mineral leaches into cooking water and gets poured down the drain with the liquid. Steam vegetables lightly until they're bright green and still slightly crisp, or sauté quickly with a small amount of healthy fat to enhance absorption.
The Salad Dressing That Steals Your Calcium
Fat-free salad dressings seem like a healthy choice, especially when you're eating calcium-rich leafy greens. But calcium absorption actually requires some dietary fat to transport across your intestinal wall — without fat, the calcium can't make the journey.

Fat-free dressings leave your calcium-rich salads virtually useless for bone building, while potentially adding sugar that creates acid-buffering calcium loss. The fat-soluble transport mechanism needs lipids to create the molecular vehicles into your bloodstream. Use a small amount of olive oil-based dressing, or add sliced avocado or nuts to provide the healthy fats needed for calcium absorption. But the timing of when you eat these healthy fats matters more than most people realize.
Why Calcium Before Bed Disrupts Sleep and
Many people take calcium supplements before bed, thinking nighttime is ideal for bone repair and rebuilding. Large doses of calcium before sleep can interfere with magnesium absorption, which is essential for muscle relaxation and quality sleep.

Poor sleep directly impacts bone health by disru hormone production, which is critical for bone formation and repair during rest. The calcium-magnesium imbalance can cause restless legs, muscle cramps, and fragmented sleep, creating a cascade of problems that ultimately weaken bones. Take calcium earlier in the day and save magnesium for evening, which promotes bothation and proper calcium utilization. This is surprisingly common, but there's an even more widespread mistake involving calcium and exercise timing.
The Exercise Timing That Wastes Calcium Supplements
The Exercise Timing That Wastes Calcium Supplements
A gym scene showing someone taking supplements immediately after a workout near exercise
Taking calcium supplements immediately after exercise seems logical — you're supporting your bones right when they need recovery. But intense exercise temporarily reduces stomach acid production and blood flow to the digestive system, severely limiting calcium absorption.

Your body prioritizes muscle recovery and temperature regulation over nutrient absorption, meaning that post-workout calcium largely gets wasted. The stress horm during exercise also temporarily impair the cellular mechanisms responsible for mineral absorption. Take calcium 2-3 hours before exercise, when your digestive system is functioning optimally and can properly process and absorb the mineral. But exercise timing isn't the only physical activity that affects calcium — there's something most daily that's even more damaging.
How Sitting All Day Drains Calcium From Bones
Extended sitting, even while dutifully taking calcium supplements, actively weakens bones through a process called disuse at need mechanical stress to maintain density — without weight-bearing pressure, they begin releasing calcium regardless of dietary intake. Just 3-4 hours of continuous sitting can trigger bone breakdown processes that exceed the benefits of most calcium supplementation.

The cellular mechanisms that build bone require physical and movement to activate. Without mechanical stress, bones essentially go into conservation mode. Stand and walk for 2-3 minutes every hour, and incorporate weight-bearing activities like walking or light resistance exercises into your daily routine. This mechanical aspect of bone health connects to a crucial nutrient partnership that most people completely overlook.
The pH Balance That Controls Calcium Destiny
Most people focus on calcium quantity while completely ignoring their body's acid-alkaline balance, which determines how calcium gets used. A diet high in acid-forming foods forces your body to use bone calcium as a buffer, regardless of how much calcium you consume daily.

Common foods like processed meats, refined grains, and sodas create metabolic acidity that can override the benefits of calcium supplementation entirely. Your body maintains blood pH within a narrow range by any means necessary — including stripping calcium from bones to neutralize dietary acids. Focus on alkalizing foods like vegetables and fruits with each meal to create an environment where calcium can actually build bones instead of just buffering acids. The final piece of this puzzle involves timing that most people get completely backwards.
Why Morning Calcium Needs Evening Preparation
Most calcium advice focuses on what you do in the morning, but optimal calcium absorption actually begins with your dinner choices the night before. Evening meals high in alkalizing vegetables create the ideal pH environment for morning calcium absorption, while acidic dinners set you waste.

Your overnight fasting period is when your body processes the acid load from dinner and either prepares for or prevents effective calcium utilization the next day. The 8-10 hour overnight period allows your body to either establish alkaline mineral reserves or deplete them, directly affecting how morning calcium gets processed. End each and avoid late-night snacking to optimize your body's preparation for calcium absorption the following morning.
The Hidden Calcium Thief in Your Medicine Cabinet
Most people over 60 take at least one daily medication What seems like good health management could be quietly undermining your bone strength. But here's what most people don't know.

Many common medications actually increase calcium loss through your kidneys. This creates a hidden drain on your bone reserves. Your body pulls calcium from bones to maintain blood leaving your skeleton weaker over time. Blood pressure medications, particularly diuretics, can flush out up to 30% more calcium than normal. Even aspirin taken daily can interfere with calcium absorption in your digestive tract. The smart approach is timing. Take calcium supplements at 2 hours away from medications, and ask your pharmacist about calcium-sparing alternatives. And the next discovery might surprise you even more.
Why Your Calcium Needs Change Every Decade After 50
It's natural to assume calcium needs stay the same throughout life. Most people take the same dose they started with years ago.
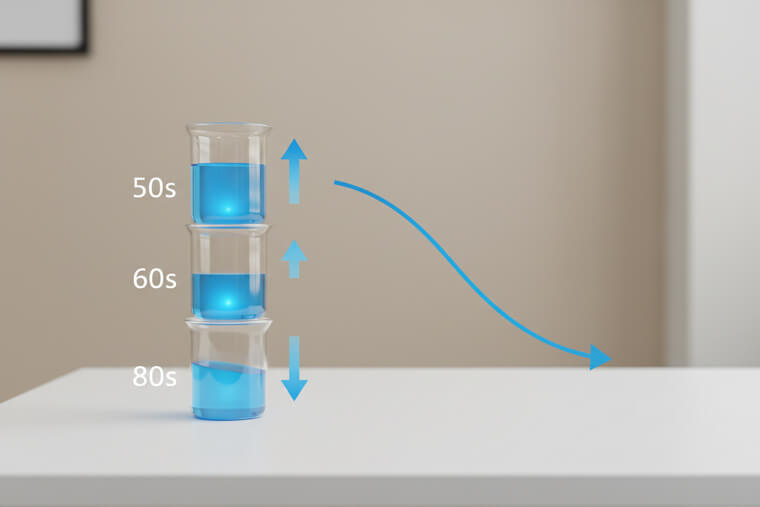
What seems logical actually works against your changing biology. Your calcium absorption drops by about 15% each decade after age 50. This means supplement dose that worked at 55 might only deliver half the benefit at 75. Your digestive system produces less stomach acid, making calcium harder to break down and absorb. The mechanism involves declining levels of stomach acid and vitamin D receptors. Your intestines literally become less efficientbing calcium from food and supplements. Smart supplementation increases gradually with age. Start with 500mg at 50, move to 800mg at 60, and consider 1000mg after 70, always split into smaller doses. The timing of when you take it matters even more than the amount.
The Water Type That Blocks Calcium Absorption
Most people drink whatever water is convenient. Staying hydrated seems like the priority, regardless of the source.

But here's what researchers discovered. Soft water can actually interf your digestive tract. This happens because soft water lacks the natural minerals that help calcium dissolve properly. Without these mineral partners, calcium can form compounds your body can't use effectively. Water softening systems remove calcium, magnesium, and other trace minerals that normally help your digestive system process bone-building nutrients. Your body ends up working harder for benefit. The better choice is filtered hard water or adding a pinch of sea salt to soft water. This provides the mineral balance your digestive system expects. But that's not the most surprising water discovery.
How Stress Hormones Steal Calcium From Your Bones
Chronic stress feels unavoidable after 60. Between health concerns, family responsibilities, and daily pressures, stress seems like just part of life.
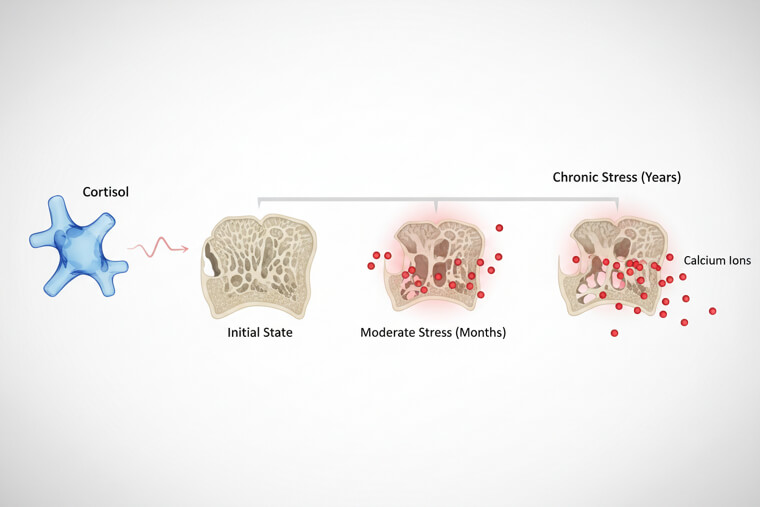
What most people don't realize is that stress hormones actively pull calcium out of bones. Cortisol literally breaks down bone tissue to access stored minerals. This creates a hidden health crisis. Even perfect calcium intake, chronic stress can override your bone-building efforts and accelerate calcium loss. The mechanism works like this: cortisol signals your bones to release calcium into the bloodstream for immediate energy needs. This emergency response becomes destructive when stress never stops. Effective stress management becomes as important as calcium supplements. Deep breathing, gentle exercise, and adequate sleep can reduce cortisol by up to 40%. The next factor affects millions but gets overlooked completely.
Why Calcium Needs Fat to Work Properly
Low-fat diets seem heart-healthy and smart for weight management. Most people over 60 try to minimize fat intake for better health.

But here's the surprising truth about calcium. Without adequate healthy fats, your body can't absorb fat-soluble vitamins that make calcium work effectively. This creates a hidden nutrition gap. Calcium depends on vitamins D, K2, and A to direct it into bones rather than soft tissues. All of these vitamins require fat for absorption. The mechanism involves bile salts that only activate in the presence of dietary fat. Without this activation, these crucial vitamins pass through your system unused, directionless. The solution is pairing calcium-rich foods with healthy fats. Add olive oil to leafy greens, nuts to yogurt, or avocado to calcium-fortified smoothies. And timing this combination unlocks even greater benefits.
The Sleep Position That Improves Calcium Absorption
Most people never connect sleep position to bone health. How you lie in bed seems completely unrelated to calcium absorption.
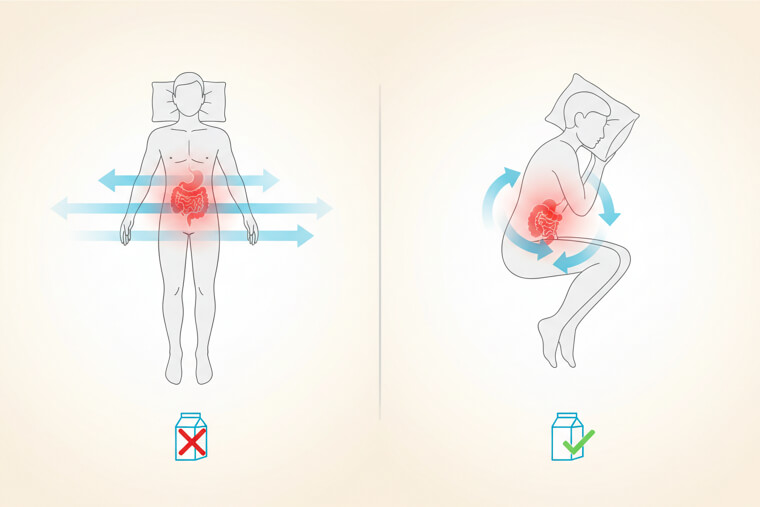
What sleep researchers discovered changes everything. Sleeping on your left side can improve digestive circulation by up to 25 the night. This matters because calcium absorption happens primarily during deep sleep phases. Better circulation means more nutrients reach bone-building cells when they're most active. The left-side position works by optimizing blood flow through your digestive organs. Your stomach and small intestine process nutrients when gravity assists rather than fights circulation. Try transitioning to left-side sleeping gradually. Use a pillow between your knees for comfort and support your arm to prevent numbness. But sleep position is just the beginning of nighttime optimization.
Why Room
Comfortable room temperature seems like a personal preference. Most people set their thermostat based on comfort rather than health considerations.

But here's what sleep scientists found. Rooms above 72°F can reduce the deep calcium absorption peaks by up to 30%. This happens because your body needs to cool down to enter the deepest sleep stages. When the environment is too warm, you spend more time in lighter sleep where bone building slows dramatically. The mechanism involves growth hormone release, which only happens during the coolest, deepest sleep phases. This hormone signals bones to absorb and utilize calcium most effectively. The optimal bedroom temperature for bone health is 65-68°F. This allows your body temperature to drop naturally and maximize growth hormone release. Most people overlook this next environmental factor completely.
The Household Chemical That Blocks Calcium Channels
Cleaning your home seems like good health practice. Using antibacterial products and sanitizers feels like protection from illness.

What most people don't know is that triclosan, found in many household cleaners, can interfere with calcium transport in your cells. This creates a hidden exposure risk. Even calcium intake, cellular transport problems can prevent the mineral from reaching bone tissue effectively. Triclosan works by disrupting calcium channels in cell membranes. These channels are essential for moving calcium from your bloodstream into bone-building cells where it's needed. Choose triclosan-free cleaning products and antibacterial soaps. Simple soap and water often work just without the calcium interference. The next discovery might be hiding in your kitchen right now.
How Aluminum Cookware Competes With Calcium
Aluminum cookware seems convenient and affordable. Most kitchens have least a few aluminum pots or pans for everyday cooking.

But here's what nutritionists discovered. Aluminum can compete with calcium for absorption sites in your digestive tract, reducing calcium uptake by up to 20%. This happens because aluminum and calcium use similar transport mechanisms in your intestines. When both are present, aluminum often wins the competition for absorption. Regular useware can lead to gradual aluminum accumulation in your system. This accumulated aluminum continues interfering with calcium absorption long after cooking. Stainless steel, cast iron, or ceramic cookware eliminates this competition. Your calcium supplements and food sources work more effectively without aluminum interference. And the next factor affects your absorption every single day.
Why Shower Water Temperature Impacts Bone Health
Hot showers feel relaxing and therapeutic. Most people use the hottest water they can comfortably tolerate, especially on mornings.

What circulation specialists found is surprising. Water above 104°F can reduce circulation efficiency for up to 4 hours after showering. This matters because calcium absorption depends on good circulation to transport nutrients from your digestive system to bone tissue. Reduced circulation means less calcium reaches where it's needed most. Hot water causes blood vessels to dilate temporarily, then constrict as your body temperature normalizes. This constriction period reduces nutrient transport efficiency throughout your system. Moderate shower temperatures (98-102°F) provide comfort without circulation disruption. End with 30 seconds of cooler water to stimulate healthy. The next environmental factor surprises most people completely.
The Light Exposure That Maximizes Calcium Utilization
Getting sunlight seems like basic health advice. Most people know vitamin D comes from sun exposure but don't understand the details.

But here's what photobiology research reveals. The angle of sunlight changes vitamin D production efficiency by up to 400% throughout the day. This matters because vitamin D directly controls how much calcium your bones can absorb and utilize. Without optimal vitamin D, calcium supplementation becomes largely ineffective. The sun's UV-B rays, which trigger vitamin D production, are strongest when your shadow is shorter than your body height. This typically happens between 10 AM and 2 PM. Spend 15-20 minutes in direct sunlight during peak hours, exposing arms and face without sunscreen initially. This maximizes vitamin D production for calcium utilization. But timing your calcium intake creates even greater benefits.
Why Electromagnetic Fields Might Disrupt Calcium Transport
Electronic devices seem harmless and necessary for modern life. WiFi, cell phones, and smart devices surround us constantly without obvious health effects research suggests is concerning.

Strong electromagnetic fields might interfere with calcium ion movement across cell membranes. This could affect how efficiently calcium moves from your bloodstream into bone-building cells. Even perfect calcium levels become less effective if cellular transport systems aren't working optimally. The mechanism involves electrical charges that calcium ions carry. External disrupt these natural electrical processes in your cells. Simple precautions include keeping phones away from your body for several hours after taking calcium supplements, and turning off WiFi routers at night during peak bone-building hours. Most people skip this next crucial timing consideration.
The Seasonal Calcium Most People Ignore
Calcium needs seem constant throughout the year. Most people take the same supplements and eat similar foods regardless of season.
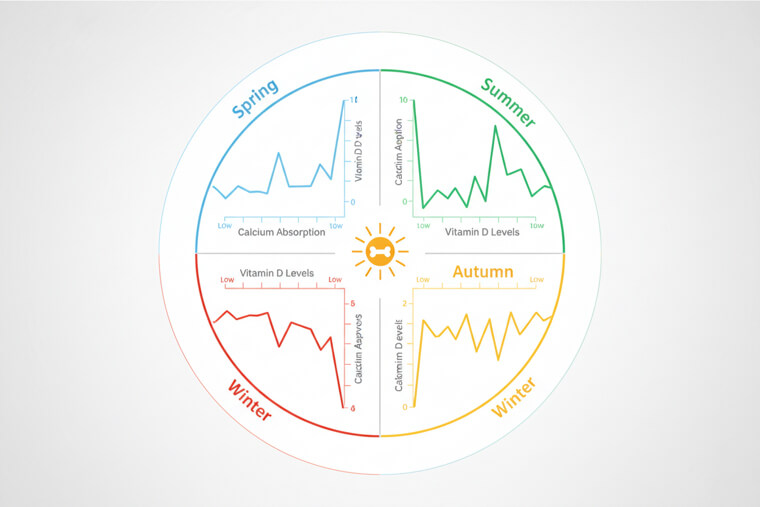
What seasonal biology reveals changes everything. Your calcium absorption can vary by up to 50% between summer and winter months. This happens because vitamin D production drops dramatically especially above 37 degrees latitude. Without adequate vitamin D, calcium absorption becomes severely impaired. The mechanism involves both sunlight exposure and seasonal changes in metabolism. Your body naturally conserves energy in winter, which can slow bone remodeling and calcium utilization. Winter calcium supplementation should increase by 25-40%, paired with vitamin D3 supplements of at least 2000 IU daily. Summer allows for reduced supplementation with increased sun exposure. The next pattern affects your calcium needs in ways you'd never expect.
How Blood Type Influences Calcium Absorption
Blood type seems relevant only for medical emergencies. Most people know their type but don't connect it to daily nutrition needs.

But here's what personalized nutrition research discovered. Different blood types can have up to 35% variation in calcium absorption efficiency. This happens because blood type affects digestive enzyme production and stomach acid levels. These factors directly impact how well your body breaks down and absorbs calcium from food and supplements. Type O individuals typically have higher stomach acid and absorb calcium more efficiently. Type A individuals often need additional digestive support or different calcium for optimal absorption. Consider calcium citrate if you're Type A or B, as it's easier to absorb with lower stomach acid. Type O individuals often do well with calcium carbonate taken with meals. And your family history reveals even more specific patterns.
The Gut Bacteria That Control Calcium Destiny
Gut health seems separate from bone health. Most people focus on calcium intake without considering digestive ecosystem balance.
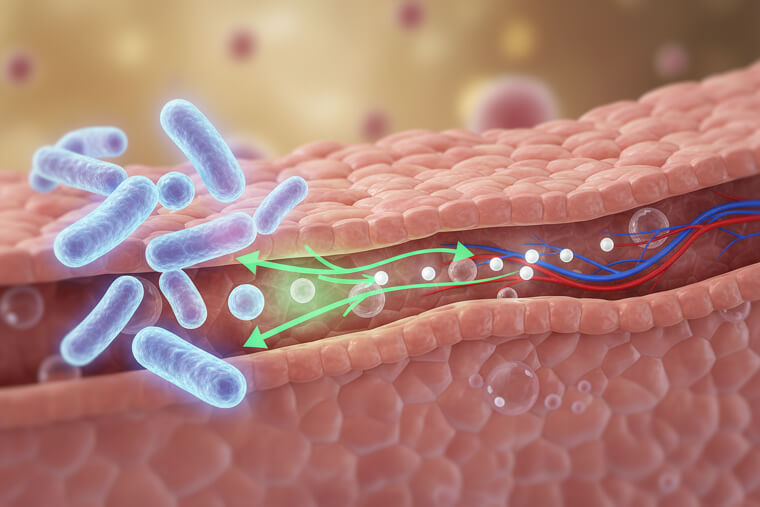
What microbiome research reveals is game-changing. Specific gut bacteria can increase calcium absorption by up to 70% when present in adequate numbers. This happens because beneficial bacteria produce enzymes that break down calcium compounds and create the ideal pH. They also produce vitamin K2, which directs calcium into bones rather than arteries. Lactobacillus and Bifidobacterium strains are particularly important for calcium metabolism. When these populations are low, calcium supplementation becomes significantly less effective. Probiotic supplements containing at least 10 billion CFU of mixed strains can restore calcium- bacteria. Fermented foods like kefir, sauerkraut, and kimchi provide ongoing support. And this brings us to the most important realization of all.
Why Calcium Timing Matters More Than Amount
Most on getting enough calcium without considering when they take it. The total daily amount seems more important than timing details.

But here's what chronobiology research proves. Your body can only absorb about 500mg of calcium at one time, regardless of how much you consume. This means taking large doses wastes most calcium and can actually interfere with absorption of other minerals. Your body literally can't process calcium efficiently in large amounts. The mechanism involves calcium transport proteins that become saturated quickly. Once saturated, additional calcium passes through your system unused or forms insoluble compounds. Divide calcium into 3-4 smaller doses throughout the day. Take 200-300mg with each meal and a final dose before bed for optimal absorption and utilization. But even perfect timing won't work without this crucial understanding.
The Calcium Cofactor Most People Never Heard Of
Calcium, magnesium, and vitamin D get all the bone health attention. Most supplement protocols focus on these three primary nutrients.

What trace mineral research discovered is shocking. Boron deficiency can reduce calcium absorption by up to 40%, even with intake of major minerals. This happens because boron regulates calcium and magnesium metabolism at the cellular level. Without adequate boron, your body can't efficiently use the calcium you're consuming. Boron activates vitamin D, helps produce estrogen and testosterone (both crucial for bone health), and enables proper calcium transport into bone tissue. Most diets provide only 1-2mg of boron daily, but optimal bone health requires 3-10mg. Prunes, almonds, and avocados are excellent sources, or consider a 3mg boron supplement. And this leads to the final piece of the calcium puzzle.
pH Balance Controls Calcium Absorption
Body pH seems like advanced chemistry with little practical relevance. Most people never think about acid-alkaline balance in daily life.
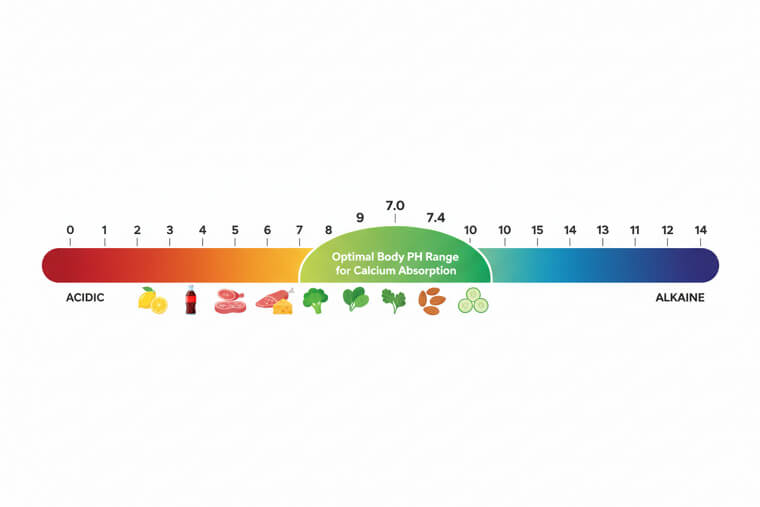
But here's what biochemistry research reveals. Your body's pH directly determines whether calcium builds bones or gets wasted through urine. This happens because calcium serves as your body's primary pH buffer. When your system becomes too acidic, it pulls calcium from bones to neutralize excess acid. The modern diet creates chronic low-grade acidosis through processed foods, excess protein, and refined sugars. This forces to sacrifice calcium for pH balance, regardless of supplement intake. Alkalizing foods like leafy greens, lemon water, and vegetables can reduce calcium loss by up to 50%. Monitor your first morning urine pH - it should be between 6. 5-7. 0. This understanding changes everything about calcium supplementation.
The Complete: Your Personal Calcium Action Plan
Everything you've learned reveals a crucial truth. Calcium absorption isn't about one supplement or one strategy - it's about creating the right conditions throughout your entire system.
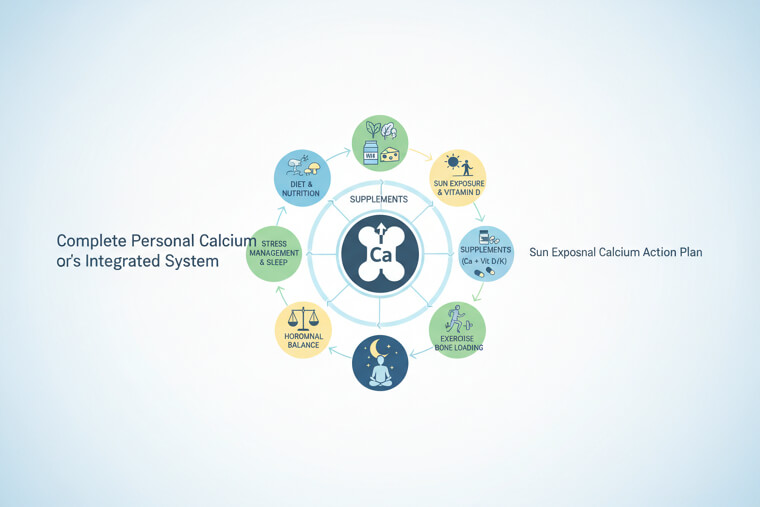
Your genetics, gut, stress levels, sleep quality, and daily habits all work together to determine how well your body uses calcium. No single factor works in isolation. This means small improvements in multiple areas create dramatically better results than focusing on calcium amount alone. Optimizing timing, cofactors, and absorption conditions multiplies effectiveness. The mechanism involves treating your body as integrated system rather than isolated parts. When digestion, circulation, hormones, and cellular transport all function optimally, calcium naturally flows where it's needed. Start with three changes: split your calcium into smaller doses, add magnesium and vitamin K2, and improve your gut health with probiotics. Build from there based on your personal response patterns's not about perfection - it's about creating better conditions for your body to do what it naturally wants to do: build and maintain strong, healthy bones for years to come. ***We hope you enjoyed the story about The Calcium-Rich Food That Actually Weakens Bones After 60. The events portrayed in this story are drawn from real-life experiences. However, names, images, and some details have been modified to protect the identities and privacy of the individuals involved.
